Switch to the mobile version of this page.
Vermont's Independent Voice
- News
- Arts+Culture
- Home+Design
- Food
- Cannabis
- Music
- On Screen
- Events
- Jobs
- Obituaries
- Classifieds
- Personals
Browse News
Departments
-
Education

Scott Official Pushes Back on Former State…
-
News

Burlington Budget Deficit Balloons to $13.1 Million
-
Education

Senate Committee Votes 3-2 to Recommend Saunders…
- Court Rejects Roxbury's Request to Block School Budget Vote Education 0
- Norwich University Names New President Education 0
- Media Note: Mitch Wertlieb Named Host of 'Vermont This Week' Health Care 0
Browse Arts + Culture
View All
local resources
Browse Food + Drink
View All
Browse Cannabis
View All
-
Culture

'Cannasations' Podcaster Kris Brown Aims to 'Humanize'…
-
True 802

A Burlington Cannabis Shop Plans to Host…
-
Business

Judge Tosses Burlington Cannabiz Owner's Lawsuit
-
Health + Fitness

Vermont's Cannabis Nurse Hotline Answers Health Questions…
-
Business

Waterbury Couple Buy Rare Vermont Cannabis License
Browse Music
View All
Browse On Screen
Browse Events
Browse Classifieds
Browse Personals
-

If you're looking for "I Spys," dating or LTRs, this is your scene.
View Profiles
Special Reports
Pubs+More
September 20, 2023 PAID POST » Health Care
How UVM Health Network – Home Health & Hospice Makes the End of Life Worth Living
Published September 20, 2023 at 10:00 a.m. | Updated September 20, 2023 at 10:10 a.m.
click to enlarge 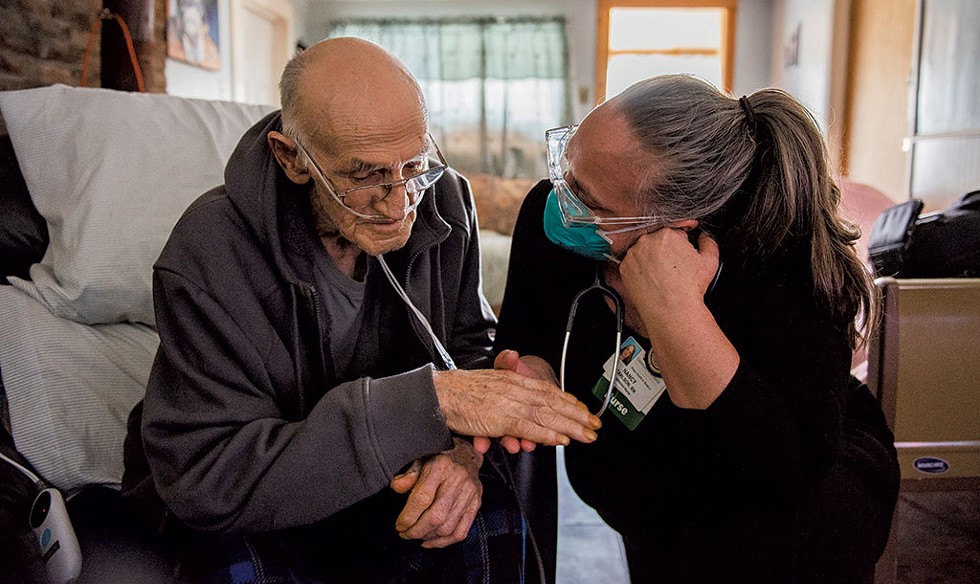

- Ryan Mercer, University of Vermont Health Network
- Nancy Carlson, RN, of the UVM Health Network – Home Health & Hospice, soothes one of her patients during a home visit
When Christine Werneke went on her first home visit to see a hospice patient in 2011, she expected it to be difficult — "I had a scary mental picture," she said. After all, hospice patients are dealing with terminal illness.
"I thought the person receiving hospice care would look very frail and fragile," she recalled.
But Werneke, now President and Chief Operating Officer of the UVM Health Network – Home Health & Hospice, said her visit wasn't anything like what she'd expected. "The patient answered the door in a muumuu, and we sat down and just had the best conversation."
As the nurse took vital signs, the three of them discussed openly and honestly how the woman was doing. "Everyone knew what was going on," Werneke said. "No one was whispering or ignoring the fact that it was a hospice visit."
"Afterward," she added, "I wanted to go on another visit."
Werneke said it's common for people to have misconceptions about end-of-life care. That's why it's so important to educate people about their options. The UVM Health Network – Home Health & Hospice program includes a highly trained, interdisciplinary team of health care professionals — and more than 300 community volunteers — who care for both the patient and the patient's family or caregivers, helping everyone navigate this transition.
Having a Support Team
Hospice is about providing care and supportive services to ensure that people get to live and die how and where they choose.
One of the most common misconceptions about it is that it's for just a few days, hospice medical director Dr. Nancy Long said: "Hospice is actually handcrafted and designed to support people for months." She often hears from patients and families who say they wish they'd known sooner how supportive it can be.
The right time to pursue hospice, she said, is when the patient is no longer seeking curative treatment. The discussion can start even sooner: The UVM Health Network – Home Health & Hospice team encourages Vermonters to talk about hospice with their provider as soon as they, or a family member, receives a terminal diagnosis. While only a medical provider can make a formal referral to hospice, patients and families can start the referral process themselves by asking their provider or doctor to contact hospice, or they can reach out directly to inquire about a referral, even if they are not sure if they are ready for hospice. An early referral gives patients the flexibility to receive hospice care either at home or at the McClure Miller Respite House in Colchester — Vermont's only Medicare-certified inpatient hospice residence — as appropriate, which can be very helpful for families (see sidebar).
Hospice social worker Tom Paquette said, "I would rather people call and ask and start the conversation, even if it's not time yet."
Paquette is part of the hospice team, too. The care team includes a physician, nurse practitioner, nurses, licensed nursing assistants, medical social workers, bereavement counselors and spiritual caregivers who are trained in working with people of multiple faiths.
Joan Newton O'Gorman, who provides spiritual care, said she often sees patients for whom relief from suffering has a spiritual connection.
In March, she was called to meet with a patient in need. When she arrived at the house, the patient's husband said she couldn't speak for herself, and he gave O'Gorman information on their faith history.
"I asked permission to say a prayer, and I held her hand, and her husband held the other," O'Gorman said. "I finished the prayer, and she died the moment I said 'Amen.' Her husband said that was the most comforting thing that could've happened."
Trained volunteers also play an integral role. Medicare requires that at least 5 percent of a hospice program's care be provided by volunteers. Most programs around the country attract a higher percentage than what Medicare requires, but the UVM Health Network – Home Health & Hospice's is particularly popular; its 300-plus volunteers — many of whom apply because they've experienced what it's like to have someone in hospice — deliver 25 to 30 percent of all care. They make meals, provide companionship, walk pets, sit vigil and bring people takeout.
"It's a remarkable volunteer program in addition to an outstanding clinical team," O'Gorman said.
At the end of life, "we need everybody, just like you do when you bring a baby into the world and we get ready for the baby," Long said. "It's not just one person. It's a team. We wrap around the family, and the person in hospice is at the center of that. We tailor our care and support services to what their goals are, knowing their time is short."
Not Giving Up
click to enlarge 

- Ryan Mercer, University of Vermont Health Network
- The Hospice team works with each patient to meet their goals for end of life. Here, Hospice Social Worker Ezra Lebowitz and Respite House Administrative Manager Maddy Sullivan-Drake review the materials given to each patient and their family.
Though hospice workers aren't seeking a cure, they're tending to patients' medical needs. When nurse Mackenzie Burnett and social worker Julie Jacob-Ochs called on Ken Wooden for his weekly hospice visit one afternoon in June, they helped him address a severe ear infection unrelated to the cancer that led him to hospice.
The infection made him uncomfortable and kept him from hearing but didn't stop the octogenarian from telling jokes and sharing his life story.
Meanwhile, Burnett contacted doctors to determine options for antibiotics and bandaged a cut on Wooden's leg. While she attended to his medical issues, social worker Julie Jacob-Ochs spoke to Wooden's wife and daughter about how they were handling the stress of the situation. She made suggestions to help them cope, such as setting up a schedule to go on walks together.
Wooden's family described him as resilient, which might have something to do with the tattoo on his arm, which he got late in life. Wooden eagerly showed it off. "You know what that says? 'Nuts,'" he said. It references his time in the army, which he said turned his life around. During the Battle of the Bulge, in World War II, he recalled, the Germans told the Americans they should surrender.
"And that's what they said: 'Nuts.' And they won the battle. They beat the Germans, and that story taught me to never give up. So that's what I do. I never, ever give up," he said.
The UVM Health Network – Home Health & Hospice team also emphasizes that hospice care is not about giving up. "Hospice is just transitioning to a more comprehensive care program for the patient," Lead Bereavement Coordinator Paul Weil said — "not just for who is dying, but for their whole family."
Wooden passed away in early July shortly after being moved to the McClure Miller Respite House. His wife, Martha, was by his side. Earlier that evening, Ken's four children and Martha had gathered in his room, playing cards, drinking margaritas, laughing and sharing memories.
Wooden's daughter, Jennifer, said she was happy her father was able to spend his last few months in his favorite place – Vermont. "That was possible because the hospice care he got here was just so incredible."
Staying By Your Side
The support hospice provides doesn't end with death. "A wonderful thing about the hospice benefit is that we are able to provide bereavement support for a year," Long said.
Postmortem care for patients is a sacred time. At the time of death, the nursing staff ensure that the body is cared for according to the patient's wishes. Loved ones are invited to participate. At the Respite House, staff and volunteers are included by lining the hall as an opportunity to honor those they care for, reflect on the residents and accompany them on their journey leaving the Respite House.
Hospice care for patients is available 24 hours a day, seven days a week. Whether in the Respite House or at home, they have access to the entire system of wraparound care to call for what they need, whenever they need it, at any time of day.
Long said she feels hospice is needed "more than ever before." Aging, sickness, dying and grief — every household experiences them. She hopes that their services can reach more of the communities they serve, she said. "The world needs us."
Providing Relief and Respite
click to enlarge 

- Ryan Mercer, University of Vermont Health Network
- Denise Barry could find day-to-day joy in her life despite the fact that she was dying. Thanks to the McClure Miller Respite House, a UVM Health Network – Home Health & Hospice service, Denise was able to receive hospice care that far exceeded anything she could get at home. This expert physical, mental and even spiritual care allowed her to live the rest of her life with dignity, comfort and celebration.
Many McClure Miller Respite House staff members skip breakfast on Thursdays because they know Mimi Hindes will bake something delicious. Both of Mimi's parents died in the Respite House. As she entered retirement, she started volunteering there alongside her husband, Church Hindes, president of UVM Health Network – Home Health & Hospice (then known as the Visiting Nurse Association) from 1999 to 2012. Mimi and Church joined the more than 300 volunteers who fulfill essential roles at the Respite House every day.
Mimi recalled when her mother became a resident. "When we walked through those doors, it was like, 'Oh, thank goodness. Someone who knows what they're doing is going to take over,'" she said. "As a family, we could start the grieving process without having to worry if Mom was in pain. The staff was wonderful."
The McClure Miller Respite House, a program of UVM Health Network – Home Health & Hospice, is named for Holly and Bob Miller and Lois McClure, longtime supporters and friends. Opened as Vermont Respite House in Williston in 1991, the residence became part of the UVM Health Network – Home Health & Hospice in 1997.
Getting it started required a tremendous volunteer effort. Back then, a residence designed for people in hospice care was a new concept. "It provided an answer for people who didn't have a caregiver at home," said Christine Werneke, the current President and Chief Operating Officer.
In the beginning, a group of community members coalesced around the idea of a Respite House. The program grew organically. In 2017, the need for more rooms drove the Respite House to move to a larger home in Colchester, funded by an $8 million fundraising campaign.
One thing that hasn't changed: No one is turned away, regardless of their ability to pay. Ongoing donations make that possible.
Every day at the Respite House is different. Staff and volunteers aid each resident in achieving their goals for end of life, support families in gathering meaningfully and mourn when residents pass away. The Respite House is a true home away from home for residents, with quilts upon each bed and home-cooked meals every day.
Church Hindes views the staff and volunteers as the "special dust" sprinkled about that make the Respite House such a sacred place: "It's always about the people who are there — a remarkable constellation of social workers and LNAs and nurses and chaplains and bereavement specialists and volunteers. The clinical teams are absolutely top drawer, truly skilled and deeply caring," he said.
This article was commissioned and paid for by Pomerleau Real Estate.
If you would like to talk to someone on the UVM Health Network – Home Health & Hospice team, call (802) 658-1900 or visit uvmhomehealth.org.




























find, follow, fan us: